GastroScholar Magazine
The Modern Journal for GI Innovation
Daily reporting on endoscopy, clinical evidence, and practice-changing advances in gastroenterology.
Editor's Picks
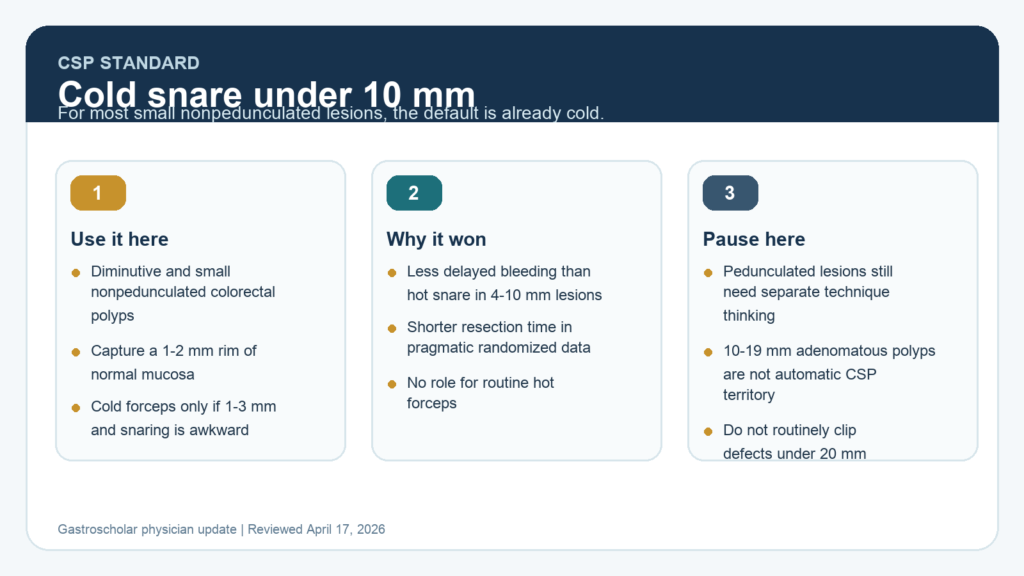
Cold Snare Polypectomy for Sub-10 mm Polyps in 2026: Where CSP Is Standard and Where It Is Not
A practical update on cold snare polypectomy for diminutive and small colorectal polyps, including technique, when hot resection is still...

EUS-Guided Gastroenterostomy for Malignant Gastric Outlet Obstruction in 2026: Where It Fits Between Stenting and Surgery
A practical clinician update on EUS-guided gastroenterostomy for malignant gastric outlet obstruction, including when it outperforms enteral stenting, when surgery...
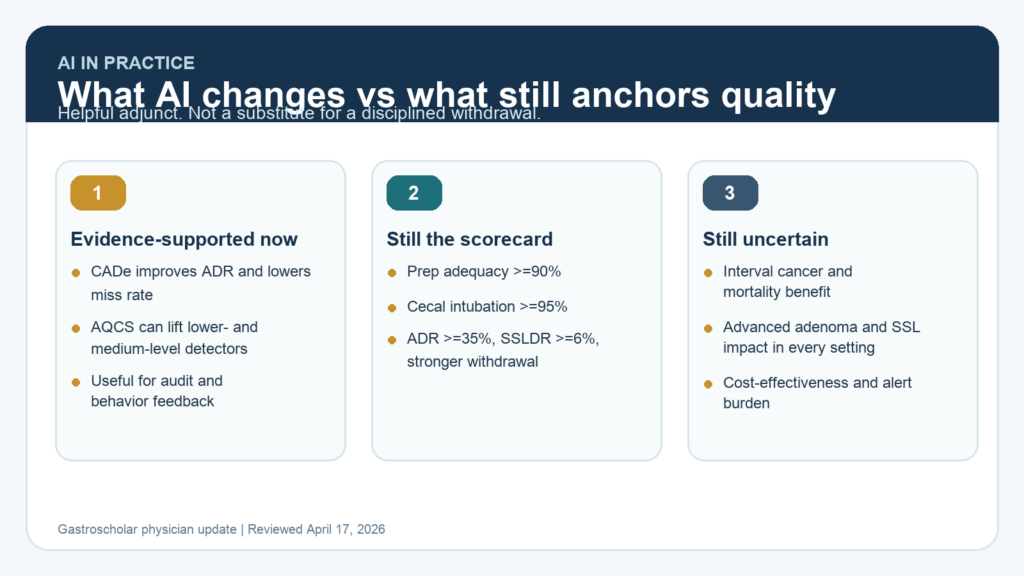

AI in Colonoscopy Quality: What CADe Changes and What Still Depends on the Endoscopist
A clinician-focused review of CADe, AI quality-control systems, and the quality indicators that still define a good colonoscopy in 2026.
Just In
-
Cold Snare Polypectomy for Sub-10 mm Polyps in 2026: Where CSP Is Standard and Where It Is Not
-
Endoscopy Sedation in 2026: Propofol, Capnography, and When Anesthesia Support Is the Safer Plan
-
AI in Colonoscopy Quality: What CADe Changes and What Still Depends on the Endoscopist
-
IBS-D Biomarkers in 2026: Positive Diagnosis, Fecal Calprotectin, and When Colonoscopy Still Matters
-
Chronic Hepatitis B in 2026: EASL 2025, Functional Cure, and What Still Belongs in Practice
-
The 2026 Frontiers: Robotic Endoscopy and Cryoballoon Efficacy
-
EUS-Guided Drainage of Peripancreatic Fluid Collections in 2026: When To Drain, When To Wait, and When Percutaneous Still Matters
-
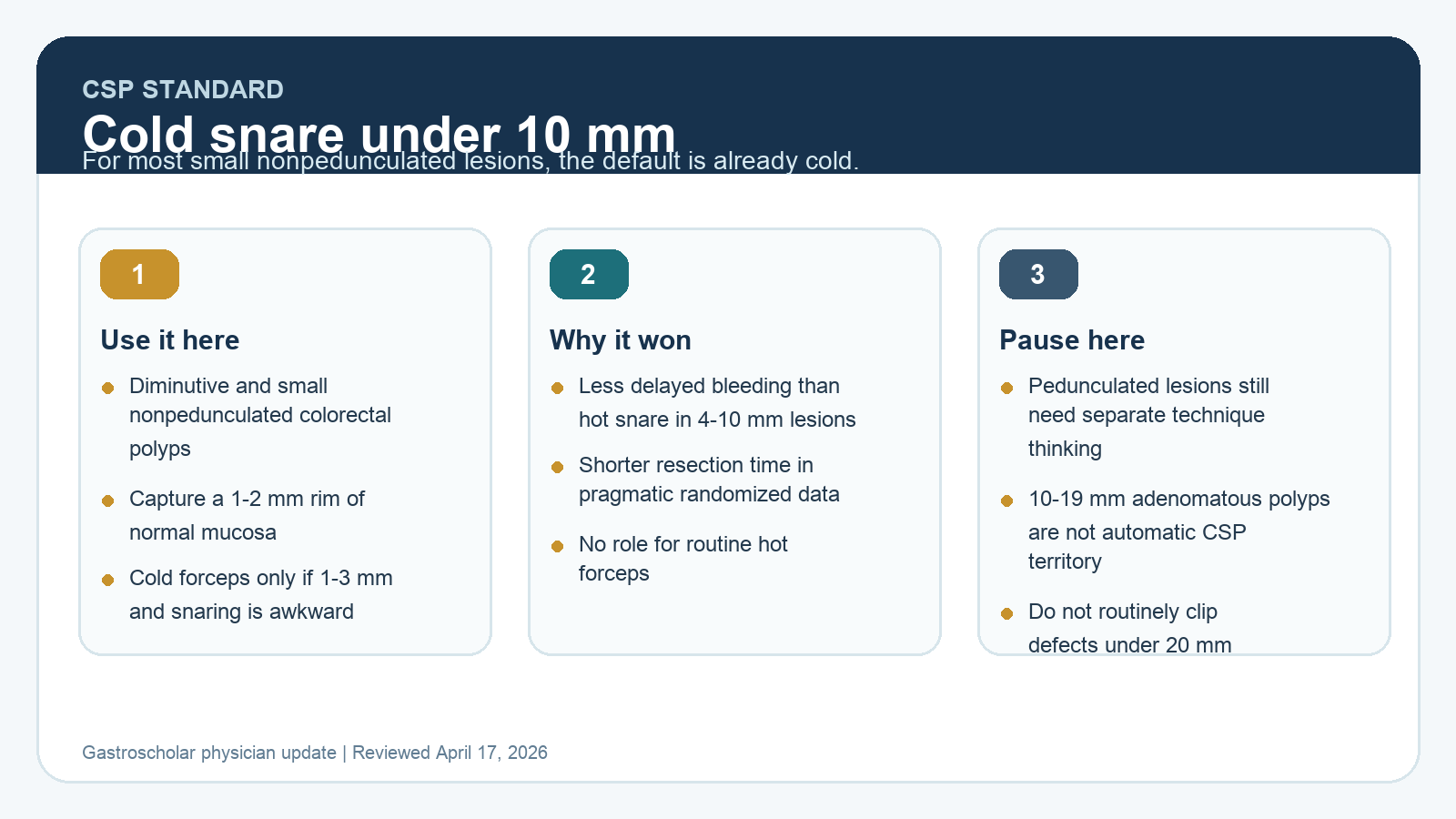
Cold Snare Polypectomy for Sub-10 mm Polyps in 2026: Where CSP Is Standard and Where It Is Not
A practical update on cold snare polypectomy for diminutive and small colorectal polyps, including technique, when hot resection is still reasonable, and what current guidelines say about clipping and forceps.
Top Stories
Trending in GI Research
-
The 2026 Frontiers: Robotic Endoscopy and Cryoballoon Efficacy
-

EUS-Guided Drainage of Peripancreatic Fluid Collections in 2026: When To Drain, When To Wait, and When Percutaneous Still Matters
-
Gastric Functional Zones: The Fundus vs. Antrum Dynamics
-
Dieulafoy’s Lesion: The Exoluminal Arterial Blowout
-
Slim Therapeutic Gastroscopes (9.2mm) in Difficult Anatomies
-
Accessories for Upper Esophageal Sphincter (UES) Interventions
Latest from the Archive
-

Deep Sedation Assessment: The Mallampati Score (2026)
Clinical Bottom Line Mallampati Class Visible Anatomy Airway Risk Profile Class I Soft palate, fauces, uvula, and pillars are completely
-
Informed Consent and Pre-procedural Optimization (2026)
Clinical Bottom Line Procedural Domain Mandatory Consent Elements Specifically Quoted Statistics Diagnostic Endoscopy Bleeding, Perforation, Sedation risks. Perforation risk generally
-

Managing Hypoxia and Airway Complications in Endoscopy
Clinical Bottom Line Intervention Step Maneuver Physiological Goal 1. Physical Stimulation Assertive sternal rub or verbal prompting. Reverses mild sedation-induced
-

Sedation Monitoring: Capnography in the ASC
Clinical Bottom Line Monitoring Modality Physiological Metric Latency to Alarm Capnography (EtCO2) Ventilation (Exhalation of end-tidal carbon dioxide). Immediate (
-

Endoscopic Infection Control: Reprocessing Standards (2026)
Clinical Bottom Line Reprocessing Stage Mechanism Vulnerability Point Pre-Cleaning Immediate bedside detergent wipe and channel flush. Failing to act prior
-
Quality Metrics in Endoscopy: ADR and Beyond
Clinical Bottom Line Quality Metric Current Clinical Benchmark Relevance to Patient Safety Adenoma Detection Rate (ADR) ≥ 25% for mixed-gender
-
Diagnostic Yield in Functional Dyspepsia (2026)
Clinical Bottom Line Patient Cohort Indication for EGD Expected Diagnostic Yield Age < 60, No Alarm Features Refractory dyspepsia defying
-
Endoscopy Masterclass: Core Modalities (2026)
Clinical Bottom Line Endoscopic Discipline Scope Architecture Functional Horizon Luminal (EGD/Colonoscopy) Forward-viewing, 120-170 degree field of view. Diagnostic mapping and
-
Pre-Endoscopy Triage: Anticoagulation and Fasting Guidelines
Clinical Bottom Line Pre-Procedural Factor Standard Metric High-Risk Variance Strict Fasting (NPO) Clear liquids up to 2 hours prior; Solids
-
Recent Advances in Upper Endoscopy (2026)
Clinical Bottom Line Technological Advance Mechanism Clinical Superiority Transnasal Endoscopy (TNE) Ultra-thin scope passed via the inferior nasal meatus. Unsedated
-
Anesthesia Paradigms: Conscious Sedation vs. MAC (2026)
Clinical Bottom Line Sedation Modality Pharmacologic Mechanism Clinical Setting / Indication Moderate (Conscious) Sedation Opioid (Fentanyl) + Benzodiazepine (Midazolam). Routine
-

Core Ambulatory Endoscopy Procedures: A 2026 Guide
Clinical Bottom Line Core Procedure Anatomical Scope Primary Clinical Indication Esophagogastroduodenoscopy (EGD) Esophagus, Stomach, Duodenum. Dyspepsia, dysphagia, GERD, Barrett’s screening,